Anatomy and Physiology of the Female Reproductive System
Anatomy of the Female Reproductive System
The anatomy of the female reproductive system consists of structures that include the external female genitals and internal female reproductive organs. They are described below.
External Female Genitals
The external female reproductive structures are referred to collectively as the vulva and include the mons pubis, the labia majora, and the labia minora.
The mons pubis is a pad of fat that is located at the anterior, over the pubic bone. After puberty, it becomes covered in pubic hair.
The labia majora (labia = “lips”; majora = “larger”) are folds of hair-covered skin that begin just posterior to the mons pubis.
The labia minora (labia = “lips”; minora = “smaller”) is thinner and more pigmented and extends medially to the labia majora. Although they naturally vary in shape and size from woman to woman, the labia minora serve to protect the female urethra and the entrance to the female reproductive tract.
The superior, anterior portions of the labia minora come together to encircle the clitoris (or glans clitoris), an organ that originates from the same cells as the glans penis and has abundant nerves that make it important in sexual sensation and orgasm. The hymen is a thin membrane that sometimes partially covers the entrance to the vagina.
The vaginal opening is located between the opening of the urethra and the anus. It is flanked by outlets to the Bartholin’s glands.
Internal Female Reproductive Organs
Vagina
The vagina is a muscular canal (approximately 10 cm long) that is the entrance to the reproductive tract. It also serves as the exit from the uterus during menses and childbirth. The outer walls of the anterior and posterior vagina are columns with ridges. The superior fornix meets the uterine cervix. The cervix is the opening to the uterus.
The walls of the vagina are lined with:
- An outer, fibrous adventitia
- A middle layer of smooth muscle
- An inner mucous membrane with transverse folds (called rugae)
Together, the middle and inner layers allow the expansion of the vagina to accommodate intercourse and childbirth. The thin, perforated hymen can partially surround the opening to the vaginal orifice. The Bartholin’s glands and the lesser vestibular glands (located near the clitoris) secrete mucus, which keeps the vestibular area moist.
The vagina has a normal population of microorganisms that help to protect against infection. There are both pathogenic bacteria and yeast in the vagina. In a healthy woman, the most predominant type of vaginal bacteria is from the genus Lactobacillus, which secretes lactic acid. Lactic acid protects the vagina by maintaining an acidic pH (below 4.5).
Lactic acid, in combination with other vaginal secretions, makes the vagina a self-cleansing organ. However, douching can disrupt the normal balance of healthy microorganisms and increase a woman’s risk for infections and irritation. It is recommended that women do not douche and that they allow the vagina to maintain its normal healthy population of protective microbial flora.
Ovaries
The ovaries are the female gonads. There are two, one at each entrance to the fallopian tube. They are each about 2 to 3 cm in length, about the size of an almond. The ovaries are located within the pelvic cavity. The ovary itself is attached to the uterus via the ovarian ligament. The ovarian stroma forms the bulk of the adult ovary. Oocytes develop within the outer layer of this stroma, each surrounded by supporting cells. This grouping of an oocyte and its supporting cells is called a follicle.
The Fallopian Tubes
The fallopian tubes are the conduit of the oocyte from the ovary to the uterus. Each of the two fallopian tubes is close to, but not directly connected to, the ovary.
- The isthmus is the narrow medial end of each uterine tube that is connected to the uterus.
- The wide distal infundibulum flares out with slender, finger-like projections called fimbriae.
- The middle region of the tube, called the ampulla, is where fertilization often occurs.
The fallopian tubes have three layers:
- An outer serosa
- A middle smooth muscle layer
- An inner mucosal layer
In addition to its mucus-secreting cells, the inner mucosa contains ciliated cells that beat in the direction of the uterus, producing a current that will be critical to moving the oocyte.
The Uterus and Cervix
The uterus is the muscular organ that nourishes and supports the growing embryo. Its average size is approximately 5 cm wide by 7 cm long, and it has three sections:
- The portion of the uterus superior to the opening of the uterine tubes is called the fundus.
- The middle section of the uterus is called the body of the uterus (or corpus).
- The cervix is the narrow inferior portion of the uterus that projects into the vagina.
The cervix produces mucus secretions that become thin and stringy under the influence of high systemic plasma estrogen concentrations, and these secretions can facilitate sperm movement through the reproductive tract.
The wall of the uterus is made up of three layers:
- Perimetrium: the most superficial layer and serous membrane.
- Myometrium: a thick layer of smooth muscle responsible for uterine contractions.
- Endometrium: the innermost layer containing a connective tissue lining covered by epithelial tissue that lines the lumen. It provides the site of implantation for a fertilized egg and sheds during menstruation if no egg is fertilized.
Physiology of the Female Reproductive System
Following ovulation, the fallopian tube receives the oocyte. Oocytes lack flagella and therefore cannot move on their own.
High concentrations of estrogen that occur around the time of ovulation induce contractions of the smooth muscle along the length of the fallopian tube. These contractions occur every 4 to 8 seconds, causing the oocyte to flow toward the uterus through the coordinated beating of the cilia that line the outside and lumen of the length of the fallopian tube which pulls the oocyte into the interior of the tube. Once inside, the muscular contractions and beating cilia move the oocyte slowly toward the uterus. When fertilization does occur, sperm typically meet the egg while it is still moving through the ampulla.
Watch this video on ovulation from MedlinePlus to observe ovulation and its initiation in response to the release of FSH and LH from the pituitary gland.
Media 10.2. Ovulation. From Betts, et al., 2013. Licensed under CC BY 4.0.
The Menstrual Cycle
The three phases of the menstrual cycle are:
- The menses phase of the menstrual cycle is the phase during which reproductive hormone levels are low, the woman menstruates, and the lining is shed. The menses phase lasts between 2–7 days with an average of 5 days.
- The proliferative phase is when menstrual flow ceases and the endometrium begins to proliferate (regrow). During this phase, reproductive hormones are working in homeostasis to trigger ovulation on approximately day 14 of a typical 28-day menstrual cycle. Ovulation marks the end of the proliferative phase.
- The secretory phase is when the endometrial lining prepares for the implantation of a fertilized egg. If no pregnancy occurs within approximately 10–12 days, the endometrium will grow thinner and shed starting the first day of the next cycle.
Image Descriptions
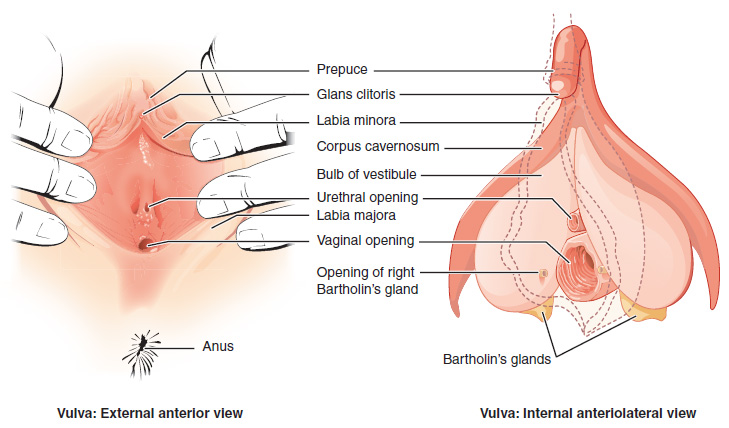
Figure 15.1 image description: This figure shows the parts of the vulva. The right panel shows the external anterior view and the left panel shows the internal anterolateral view. The major parts are labeled (from top): prepuce, glans clitoris, labia minora, corpus cavernosum, bulb of vestibule, urethral opening, labia majora, vaginal opening, opening of right Bartholin’s gland, Bartholin’s glands, anus. [Return to Figure 15.1].

